Treating children who are unwell can be challenging. It’s especially difficult for a child and their family when childhood cancer is diagnosed.
Treatment for paediatric cancers is often complex and intensive, but thanks to considerable investment in research over the last 50 years, they are a lot more treatable than they used to be, and cure rates in children are high.
According to Cancer Research UK, children’s cancer survival in the UK has more than doubled since the 1970s, and now 85% of children treated for cancer live five years or more, and many fully recover.
As more children and young adults survive cancer, the impact of any treatment becomes more important, and doctors are constantly looking for evidence of treatments that are less invasive and more targeted.
Proton beam therapy (PBT) is today proving critical in this area, and here we look at its role as a paediatric cancer treatment.
Why is proton beam therapy considered beneficial for treating cancers in children and young people?
When cancer is diagnosed in young patients, there are a variety of treatments that paediatric consultants might consider, but generally, they will include surgery, chemotherapy or radiotherapy or a combination of these. Proton beam therapy is a type of radiotherapy.
Children’s and young people’s bodies are not just smaller than adults – they are still growing and changing, and because of this, there is evidence that certain types of cancer treatment can have a detrimental impact on their adult life years after the treatment has finished.
Late effects of radiotherapy are particularly high in children and young people due to the vulnerability of growing tissues, and so where possible, doctors will try to find an optimal treatment which will cure the cancer and also have minimal effect on a child’s development.
What is the difference between proton beam therapy and radiotherapy?
We already know that traditional radiation therapy (also termed radiotherapy) is proven to be effective in the treatment of many cancers, and new methods of delivering it mean that it can be more targeted than ever before.
Photons
Very simply put, conventional photon radiotherapy delivers beams of photons (x-rays) to a tumour to damage the cancerous cells until they can’t divide anymore and die.
Photons can be delivered in a precisely targeted way with intensity-modulated radiotherapy (IMRT), effectively killing cancer cells. However, the beams continue through the body, also damaging healthy cells in their wake – this is the exit dose.
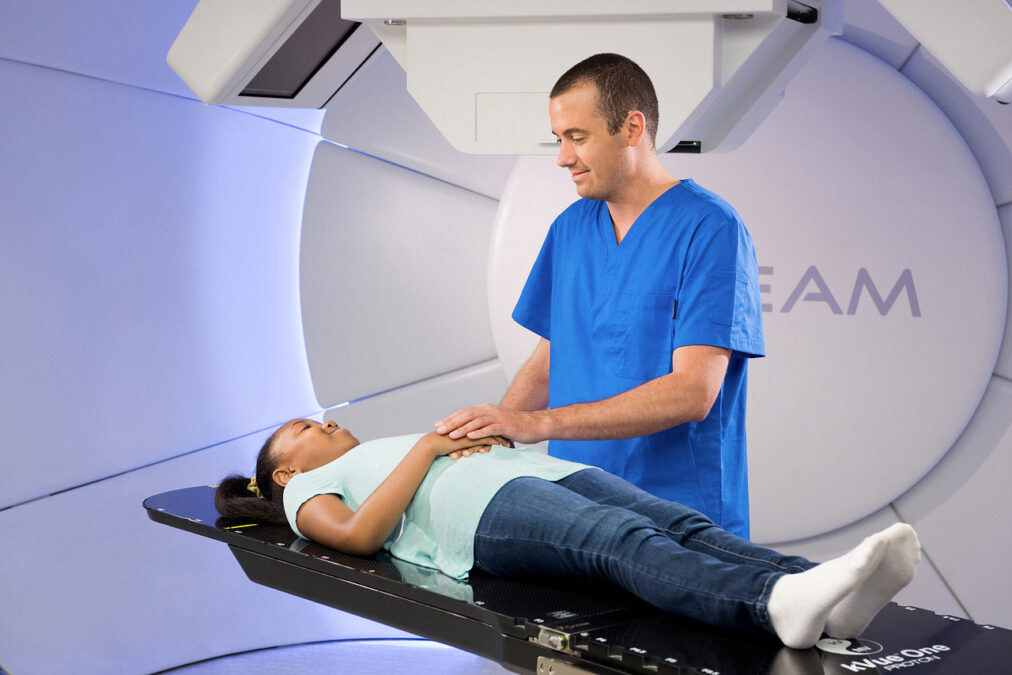
Protons
Proton beam therapy (PBT) offers another tool in the armoury of radiation oncology, allowing paediatric radiation oncologists to precisely target individual tumours but without an exit dose.
Radiation oncologists can manipulate protons, which are small parts of atoms, to stop at the site of the tumour and do the damage required to kill the cancerous cells and only those. In turn, this generally means fewer damaging effects and toxicities on surrounding healthy tissue during and after treatment.
In many cases, PBT offers an equivalent chance of cure to conventional photon radiotherapy, but there is a theoretical reduction in both short- and long-term side effects.
The greater precision PBT allows, including intensity modulated proton therapy (IMPT) which uses pencil beam scanning (PBS) minimises damage to surrounding healthy cells, which is especially useful in the treatment of cancers in children.
When treating a child or young person, it makes sense to minimise radiation exposure and avoid as much damage as possible to surrounding healthy tissue.
Is proton beam therapy available in the UK?
There is a mix of both private and NHS-funded proton beam therapy treatment available in the UK: The Christie Hospital in Manchester treats NHS patients, and UCLH offers treatment to both NHS and private patients through Proton International London. The two centres collectively accept about 650 NHS patients (both adult and children) each year.
Globally, PBT is not as available as perhaps most paediatric oncologists would like and until fairly recently, UK patients had to travel abroad to receive treatment. The NHS has been sending selected patients abroad for PBT since 2008. Now it is available in the UK, it is hoped that PBT could be offered more widely than previously.
If you would like to find out more, contact us today.
Is proton beam therapy suitable for all paediatric cancers?
No, not all children will be suitable for proton therapy treatment, nor is it the right treatment for all paediatric cancers. For a variety of clinical reasons, other cancer treatments might be considered better options.
If you think your child might benefit from PBT, you should discuss it with your paediatric oncologist, who will help you make an informed decision and can refer you to a radiation oncologist that specialises in paediatric PBT.
What types of childhood cancers can be treated with proton therapy?
The cost and limited availability of PBT mean clinicians have to be very selective about which patients will benefit the most from it, and children are often a priority.
PBT can be used to treat a variety of paediatric cancers. The following list is not exhaustive, but the cancers include:
- Brain/central nervous system cancers (CNS) including glioma, medulloblastoma, ependymoma, atypical teratoid/rhabdoid tumour, craniopharyngioma, germ cell tumour.
- Sarcomas, including chordoma/chondrosarcoma, Ewing sarcoma, osteosarcoma, rhabdomyosarcoma and others.
- Neuroblastoma.
- Wilms tumours.
- Spinal cord tumours.
- Lymphomas, including Hodgkin and non-Hodgkin lymphoma.
- Cancers in the head and neck, including parotid gland, nasopharyngeal and others.
- Cancers affecting the eye, such as retinoblastoma.
To date, in the UK, much of the focus for PBT has been on localised cancer tumours (cancers that have not yet spread in the body beyond the primary tumour site).
Cancers in parts of the body that are most sensitive to radiation exposure, such as in the brain, spinal cord, head and neck, where long-term damage could be caused and seriously impact a child’s future life chances and well-being, are especially likely to benefit from PBT, although cancers in all sites of the body can be considered for PBT.

Preparing a child or young person for PBT treatment
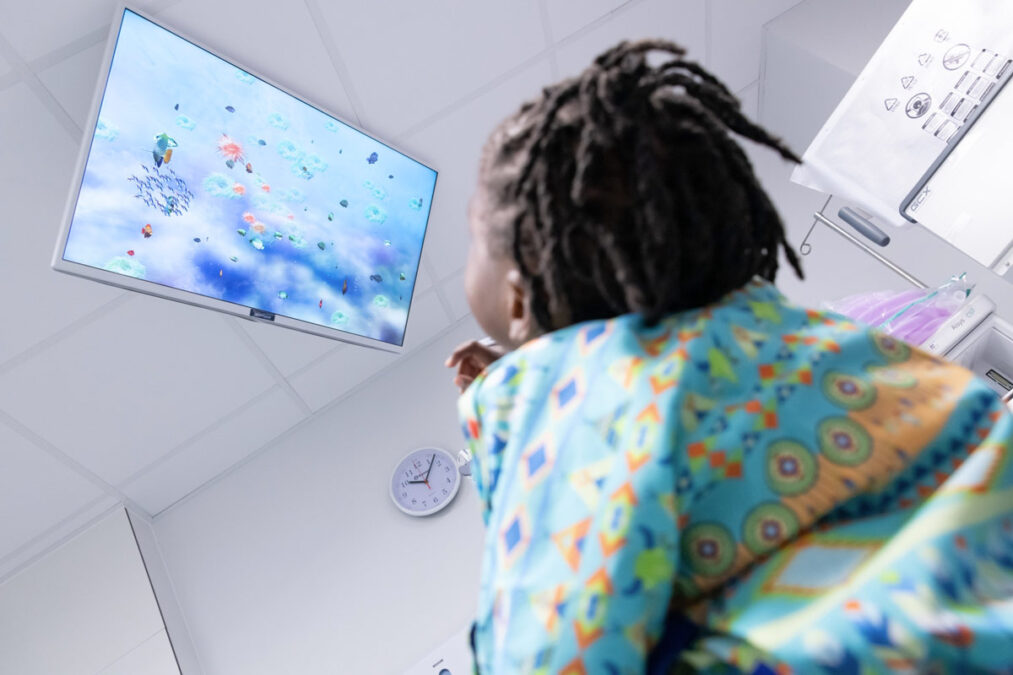
To minimise fear and worry, most PBT clinical teams use a play team who are there to reduce anxiety and help your child through the ordeal.
Play is a valuable way of helping a child understand what will happen to them, and it helps them feel comfortable with the proton beam therapy treatment.
The play specialists will help your child to understand the treatment process by experiencing elements of the treatment through play and visits to the department before treatment starts, which will help your child to become familiar with it and with the staff.
A play specialist can attend treatment appointments with your child to offer full support and guidance. They will also provide activities to keep children happy and engaged.
Will my child need to stay away from home during treatment?
A radiation oncologist specialising in paediatric cancers will prescribe your child a course of proton beam therapy over several weeks. This dose is then broken down into smaller daily doses called fractions, which are usually delivered for five consecutive days, followed by a two-day break at weekends. Treatment will usually take around 4-6 weeks.
This can present logistical challenges for families who don’t live nearby or even abroad. Parents or carers that live within travelling distance may choose to travel to the centre daily for treatment. For others who live further away, this is obviously not practical.
Most PBT centres can advise or help families arrange travel and suitable accommodation while their child is being treated. At Proton International London, we offer families a variety of places to stay within easy travelling distance of the PBT centre at UCLH.
Can I be with my child while they are receiving treatment?
Your child will need to be alone in the proton beam therapy room while they receive the treatment. Trained clinical staff will do all they can to make sure the children in their care are safe and will be monitored and well cared for at all times.
For older children and young people, the team will adapt this approach to become more age appropriate. This often takes the form of an educational session which helps them feel involved in their care.
Play specialists can also help with siblings and family members so they feel supported too.
Will my child be put under anaesthesia for PBT?
As with other forms of radiation therapy, children need to stay as still as possible when the treatment is administered. This can be difficult, especially for younger children, and so in some circumstances, a child will be given a general anaesthetic as a way of keeping them still.
In summary
Cancers in young babies, children, teenagers and young adults’ cancer present a unique set of problems for treatment because their bodies are developing and growing. Being able to closely target tumours and spare critical organs and normal tissue structures is essential to prevent the detrimental impact of treatment on their ongoing development and future life quality.
Late effects of radiotherapy are common and may manifest months to years after therapy. The great theoretical advantage of PBT, compared to conventional radiotherapy, is the reduction in collateral damage to normal tissue structures. This is especially important in young patients.

This article has been clinically reviewed by Proton International Medical Director and Consultant Clinical Oncologist, Dr Beatrice Seddon. Dr Seddon specialises in the use of radiotherapy (including proton beam therapy) and chemotherapy for the management of soft tissue and bone sarcomas.





